COVID-19
Outlook for COVID-19 in 2022
Due to the rise in vaccinations and the production of antiviral pills, medical experts anticipate COVID-19 will likely lose its “pandemic” status this year. COVID-19 will likely overlap with flu season moving forward, and COVID-19 boosters are thought to mimic an annual flu vaccine.
Source: Cory Stieg. “The Pandemic Could End in 2022 — Here’s What “Normal” Life Might Look Like Soon, According to Medical Experts,” CNBC, 2021.Requirements for Insurers to Cover At-Home Over-the-Counter COVID-19 Test
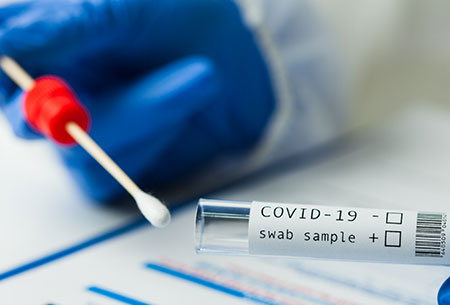
Since January 15, insurance companies have been required to cover eight at-home over-the-counter (OTC) COVID-19 tests per month. These tests can be purchased all at once or throughout the 30-day period. The allowance is for eight tests per individual on the plan. For example, a family of four on the same plan can receive thirty-two tests per month. It is important to note that plans are required to cover eight tests per month regardless of how they are packaged and distributed. Plans are encouraged to cover the cost up front for the tests by setting up a network of convenient options (e.g., pharmacies, retailers and online retailers). When doing this they can limit the test reimbursement amount for retailers outside of that network to no more than $12. However, if the plan or insurer does not set up a system to cover costs upfront, then they must reimburse the full cost of the test even if the test costs more than $12 (e.g., individual buys two-pack of tests for $34, then the plan or insurer must reimburse the $34 instead of $24 if they had set up network). Plans or issuers are not required to provide coverage for athome OTC COVID-19 tests purchased before January 15. This policy is limited to OTC COVID-19 tests purchased for individual use, and it does not extend to workplace testing
Source: Cory Stieg. “How to Get Your At-Home Over-the-Counter COVID-19 Test for Free,” CMS, 2022.Vaccine Mandate for Large Employers Blocked by Supreme Court
Originally, the Occupational Safety and Health Administration’s (OSHA) Emergency Temporary Standard (ETS) required employers with more than 100 workers to have their workers get vaccinated or tested every week. However, several Republican states filed lawsuits against the Biden administration over the vaccine-or-test mandate, stating the mandate was unconstitutional. In addition to the lawsuits, the Supreme Court listened to oral arguments on the administration’s vaccination rules, and the court’s conservative majority seemed uncomfortable with the OSHA requirement. The main argument was that OSHA could regulate occupational dangers, but it does not have the power to regulate public health more broadly. Therefore, the Biden administration’s COVID-19 vaccine-or-test requirement for large employers was blocked by the Supreme Court. However, workers at federally funded health care facilities will have a similar mandate that will remain in place, due to the facilities that receive Medicare and Medicaid funds. Lastly, even though the mandate has been blocked, individual employers are still legally allowed to mandate vaccines for their employees.
Sources: Oriana Gonzalez. “Supreme Court Blocks Biden’s Vaccine Mandate for Large Employers,” Axios, 2022.AccessDx: COVID-19 Testing in the Workplace
Although the Supreme Court blocked the OSHA standard, many employers desire to maintain employee testing procedures in their workforce. We have identified a partner in the team at AccessDx who has products available to support employers with solutions tailored to their specific needs. AccessDx can help with both workflow management and compliance through their software plus services, as well as with employee testing and the associated logistics
Sources: COVID-19 OSHA NFPAccessDx Employer Compliance Solution
Everything employers need for a compliance program.
- Multiple testing options, test supplies sent directly to preferred location (office or employee’s home)
- Proctored testing available via telemedicine, with results captured via HIPAA-compliant portal (powered by PROVENTM)
- Validation of vaccinated employee status
- Management toolset for program administration and compliance reporting
Pricing Options
- Employer Compliance Solution, including weekly rapid (antigen) testing – $99 per testing employee/month
- Employer Compliance Solution, including weekly laboratory PCR testing – $180 per testing employee/month
- Vaccinated Employee Enrollment and Validation – one-time enrollment fee of $20 per vaccinated employee
- No Additional Charges for Tested Employees who subsequently elect to vaccinate
For more information on ways AccessDx can support your testing compliance program contact OSHAPrep@accessdxlab.com

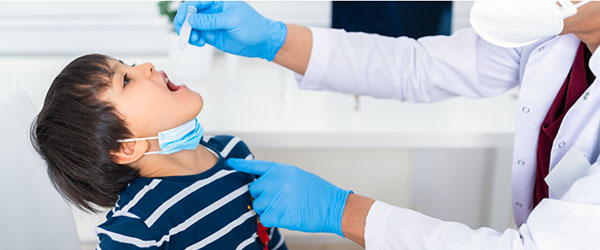
New Oral Antiviral COVID-19 Treatments: Paxlovid and Molnupiravir (Renamed Lagevrio)
As the COVID-19 pandemic continues to stress the healthcare system in the United States, one goal has been to find ways to keep people out of the hospital. With some recent emergency use authorizations (EUA) by the FDA, we may be one step closer. Two new oral antiviral drugs were granted EUA at the end of December 2021.
Pfizer’s Paxlovid combination treatment was given EUA first, followed by Merck’s molnupiravir. (Note: Merck’s has renamed molnupiravir to Lagevrio). Both medications are available only with a prescription and limited to people (at least 12 years old for Paxlovid or 18 years old for molnupiravir) who have tested positive for COVID-19 and are at greater risk for a severe disease that could lead to hospitalization or death. This means that not all who test positive for COVID-19 will be eligible to receive these medications. The CDC has organized a list of conditions that enhance the risk for a person to get severely sick from COVID-19. This list includes many chronic diseases plus those with a weakened immune system, such as transplant recipients, cancer patients and adults over 65 years old.
There are some additional limitations to using these medications, even for those who are eligible for treatment. The primary hurdle for many will be finding a location that can dispense them. The federal government has purchased around 65,000 treatment courses of Paxlovid and 300,000 courses of molnupiravir. The treatments are being allocated to states who will then further decide how to distribute the treatments. This process will vary by location but may include a mixture of clinics, hospitals, local health departments and pharmacies. Secondly, there are concerns of potential drug interactions with Paxlovid and possible birth defects with molnupiravir.
These medications are not a replacement for vaccines and are not to be used for the prevention of COVID-19 before or after suspected exposure. They are only to be used to reduce the severity of the disease, with the primary goal being to keep people from being hospitalized for treatment. To be most effective, treatment with one of these drugs needs to be started right away after a COVID-19 diagnosis and within five days of symptoms first showing.
Sources: Scott Hensley. “First Doses of Paxlovid, Pfizer’s New COVID Pill, Are Released to States,” NPR, 2021.“Coronavirus (COVID-19) Update: FDA Authorizes Additional Oral Antiviral for Treatment of COVID-19 in Certain Adults,” FDA, 2021.
“Coronavirus (COVID-19) Update: FDA Authorizes First Oral Antiviral for Treatment of COVID-19,” FDA, 2021.
“People with Certain Medical Conditions,” CDC, 2021.
Sydney Lupkin. “The COVID Antiviral Drugs Are Here but They’re Scarce. Here’s What to Know,” NPR, 2021.
Inexpensive Antidepressant may Prevent Severe COVID-19
Fluvoxamine (Luvox) is an inexpensive antidepressant showing promise in reducing the severity of COVID-19 when taken at the first signs of symptoms. Studies indicate that Fluvoxamine could decrease hospitalizations by two-thirds and deaths by 91%. Fluvoxamine belongs to a class known as selective serotonin-reuptake inhibitors (SSRIs) and was first approved by the FDA in the early 1990s. Unlike other SSRIs such as Zoloft, Fluvoxamine interacts strongly inside the cells of the body that help to regulate the body’s inflammatory response. The cost of Fluvoxamine is around $4 per treatment course and is readily available, making it a very cost-effective treatment option for COVID-19. This medication may be of particular importance in areas where vaccination rates remain low.
Sources: Maggie Fox. “Cheap, Generic Anti-depressant May Reduce Severe COVID-19 Disease, Study Finds,” CNN, 2021.Jim Dryden. “Antidepressant May Prevent Severe COVID-19, Follow-up Study Indicates,” Washington University School of Medicine in St. Louis, 2021.
“Studies indicate that Fluvoxamine could decrease hospitalizations by two-thirds and deaths by 91%.”
Drug Updates
Aduhelm Cost Decrease
In June 2021, the FDA approved a new drug, Aduhelm (aducanumab), to treat Alzheimer’s disease. There was a lot of buzz around Aduhelm when it was approved, mostly because it became the first drug that changes the underlying course of Alzheimer’s, rather than only addressing the symptoms. However, it is not a cure. Originally the cost was announced to be approximately $56,000 per year. This cost, combined with unproven clinical outcomes, and the possibility of serious side effects, including brain bleeding, lead to controversy and ultimately slow market uptake.
Biogen, the maker of Aduhelm, has expressed disappointment in the utilization of the drug since its release in 2021. They’ve made the decision to reduce the annual list price from $56,000 to $28,000 as of January 1, 2022, after considering the financial concerns for many potential patients.
Many payers are waiting for a coverage determination to be finalized by the Centers for Medicare and Medicaid Services (CMS) since a majority of the nearly 6 million Alzheimer’s patients in the U.S. are 65 and older, making them eligible for the government funded insurance. Early reports from CMS indicated that they were considering their largest increase in premiums due to the potential of covering Aduhelm, which may have been a factor in Biogen’s price reduction as well. The current CMS proposal includes covering Aduhelm but is limited to patients who are actively enrolled in clinical studies so that they can continue to collect information on the clinical impact and side effects. A final decision is tentatively due mid-April 2022.
Sources: Bob Herman. “Medicare Proposes Covering Controversial Alzheimer’s Drug, with Restrictions,” Axios, 2022.Jacob Bell. “After intense pushback, Biogen to cut price of Alzheimer's drug,” BioPharma Dive, 2022.
Jonathan Gardner and Jacob Bell. “Medicare Proposes to Limit Coverage of Biogen Alzheimer’s Drug,” BioPharma Dive, 2022.
FDA Approves Cyltezo, the First Interchangeable Biosimilar to Humira
The FDA granted interchangeability status to Cyltezo on October 15, 2021. The interchangeability designation allows for automatic substitution similar to the process allowed for traditional brand and generic drugs today. The drug will have one year of exclusiveness upon launch during which the FDA cannot grant interchangeable status to any other Humira biosimilar. Currently, Cyltezo is approved for eight out of Humira’s eleven indications.
- Adults with moderately to severely active rheumatoid arthritis
- Adults with active psoriatic arthritis
- Adults with active ankylosing spondylitis
- Adults with moderately to severely active Crohn’s disease
- Adults with moderately to severely active ulcerative colitis
- Adults with moderate to severe chronic plaque psoriasis who are candidates for systemic therapy or phototherapy and when other systemic therapies are medically less appropriate
- Pediatric patients at least 2 years old with moderately to severely active polyarticular juvenile idiopathic arthritis
- Pediatric patients at least 6 years old with moderately to severely active Crohn’s disease
Cyltezo is one of only two interchangeable biosimilars approved, Semglee (insulin glargine) being the other. Gaining interchangeable status allows pharmacies to dispense Cyltezo for Humira without having the prescriber change the prescription (subject to state pharmacy laws). Cyltezo will be offered as a single-dose, pre-filled glass syringe and administered under the skin.
Sources: Angela Maas. “FDA Grants Interchangeable Status to Humira Biosimilar, but Certain Factors May Hamper Its, Other Adalimumabs’ Uptake,” MMIT, 2021.“FDA Approves Cyltezo, the First Interchangeable Biosimilar to Humira,” FDA, 2021.
Legislation
Compromise on Lowering Prescription Drug Prices
Democrats reached an agreement to allow Medicare to negotiate pricing on some prescription medications. According to Senate Majority Leader Charles E. Schumer (D-N.Y.), “This deal will directly reduce out-of-pocket drug spending for millions of patients every time they visit the pharmacy or doctor.” However, the Medicare negotiation plan is more limited than many had hoped.
The final plan would allow Medicare to negotiate prescription drug prices for medications that are no longer protected from competition while they are still new to the market, the exclusivity period. In 2025, negotiations would begin with a group of 10 medications. For nine years, most drugs would be excluded from negotiation. Biologics, or pharmaceuticals derived from living cells, would receive a 12-year extension. After those periods of time, Medicare pricing would go into effect.
“This deal will directly reduce out-of-pocket drug spending for millions of patients every time they visit the pharmacy or doctor.”
Furthermore, prescription drug expenses for seniors would be set at $2,000 per year. Insulin will be negotiated, and out-of-pocket payments will be restricted to $35 per month. This move is likely to be politically popular given the commonly used drug’s recent and substantial price increases. It will also provide a means for seniors to spread the cost of their prescription drugs over the course of the year rather than paying it all at once.
The plan also limits the amount that drugmakers can raise their prices year after year. If the price of a drug rises faster than inflation, the manufacturer will be required to pay a rebate, a concept that authorities hope would encourage the pharmaceutical industry to keep costs low. The rebate requirement would apply to Medicare and commercial insurance plans, affecting millions of people in the United States. Lastly, drugmakers will be subject to an excise tax if they do not participate in negotiations.
Source: Jennifer Haberkorn. “Democrats Reach Deal on Medicare Prescription Drug Prices in Social Spending Bill,” Los Angeles Times, 2021.Pharmacy Chains Held Liable for Opioid Crisis
After a six-week trial, a 12-member federal jury found that three of the country’s biggest drug store chains, CVS, Walgreens and Walmart are liable for contributing to the opioid epidemic in two Ohio counties. This is considered to be the first time the retail part of the drug industry is being held accountable for the opioid epidemic.
The Ohio counties are arguing that these pharmacy companies created a public nuisance by enabling the opioid crisis. According to the Wall Street Journal, “Each county said the crisis cost them about $1 billion in expenses related to law enforcement, social services and courts.” A federal judge will decide in the spring how much the pharmacies must pay in damages. Spokesmen from these pharmacy chains have stated they strongly disagree and plan to appeal. They contend their pharmacies never manufactured/marketed opioids nor distributed them to the “pill mills” and internet pharmacies that fueled the crisis.

