Mental Health News
"TikTok Brain" Amongst the Youth
TikTok is one of the most popular social media platforms in the world. So, it’s no surprise that children and teens spend plenty of time scrolling through the app. However, because of this, health professionals, educators and parents have noticed an alarming trend regarding children’s ability to focus for extended periods.
Though research on TikTok’s usage is still limited, attention spans appear to be declining, and experts think applications like TikTok are to blame. Jessica Griffin, PsyD, an associate professor of psychiatry and pediatrics at the University of Massachusetts Medical School, stated, “Although we don’t yet have longitudinal research, there is no question that TikTok affects the brain, and children’s brains are still developing into their early to mid-twenties.” Studies indicate that technology, in general, can cause damage to youths’ impulse control and the capability to value delayed gratification.
Griffin further explained, “Short videos, like candy, provide a rush of dopamine, a feel-good chemical that’s released in the pleasure center in our brains. That rush often leaves you wanting more, like kids in a candy store.” Unfortunately, this satisfying surge makes it harder for young people to step away from TikTok and move to more productive activities. A 2021 study by NeuroImage examined China’s TikTok equivalent, Douyin, and its effects on Chinese college students’ brains. Brain scans completed on the students who used the app frequently revealed that some students lacked the self-control to stop watching.
Griffins added, “If you are watching TikTok for long periods of time, it may lead to problems with attention, concentration and short-term memory.” She also stated that other social media platforms could cause some of these same challenges for young people. These challenges include reduced real-life interactions that can lead to stunted emotional and social development.
So what can parents do? Kathryn Smerling, Ph.D., LCSW, noted that while outright banning kids from using the app isn’t a realistic or productive approach, parents who want to protect their kids from “TikTok Brain” should speak openly with their kids about the potential harms. They should also encourage them to fill their time with a range of different activities. Another option for parents is to utilize TikTok’s screen time management tool. This tool allows users to cap a time that can be locked behind a four-digit passcode.
Sources: Mira Miller. “Is 'TikTok Brain' Affecting Kids?,” Verywell Health, 2022.
The Time Is Now — Anxiety Screenings for Children
The US Preventive Task Force has noted a worsening state of mental health among children. As part of its newly drafted guidelines, the task force now recommends screening for anxiety in all children ages 8 to 18. The guidelines are open to public comment but will most likely be finalized later this year.
Anxiety is one of the most common mental health disorders among children and can go undetected for a long time. Dr. Jennifer havens, chair of Child and Adolescent Psychiatry at NYU Grossman School of Medicine, explains, “It can be quiet. Kids who are anxious are often very self-conscious and aren’t going to share this with their families or their physicians, necessarily. So screening is a very, very good idea.”
According to a report from the Child Mind Institute, childhood anxiety disorders have been linked to an increased risk for later depression, anxiety, behavior problems and substance abuse. “It’s critical to be able to intervene before a life is disrupted,” said Martha Kubik, a member of the task force and a professor in the School of Nursing at George Mason University in Fairfax, Virginia.
Usually, primary care physicians complete the majority of anxiety screenings. They use several different surveys and questionnaires that parents and/or children (depending on their age) answer. These screenings should ideally be completed during a child’s annual visit, but clinicians should also be open to opportunities to screen during other visits.
It is important to note that it is not a diagnosis if a screener indicates a child needs additional support, but more of a starting point for a bigger conversation. Experts say that the goal of these screenings is more to help doctors and other providers identify at-risk kids early on. By doing this, children can be treated before their symptoms or illness escalates.
This is not the first time this recommendation has been suggested. The American Academy of Pediatrics (AAP) has already recommended screening teens for emotional and behavioral problems like anxiety and depression. In the fall of 2021, the AAP, the American Academy of Child and Adolescent Psychiatry and the Children’s Hospital Association issued a statement calling children’s mental health a national emergency.
Sources: Christina Caron. “All Children 8 and Older Should Be Screened for Anxiety, US Task Force Says,” The New York Times, 2022.Rhitu Chatterjee. “It’s Time to Screen All Kids for Anxiety, Physicians’ Task Force Recommends,” NPR, 2022.
Brianna Abbott. “Children as Young as 8 Should Be Screened for Anxiety, Experts Recommend,” The Wall Street Journal, 2022.
The Mental Health Crisis Among US Teens
Although COVID-19 intensified the mental health decline in teenagers, this has been a widespread issue well before the pandemic hit. The US Surgeon General previously warned of a “devastating” mental health crisis among adolescents. It has been called a national emergency by many hospital and doctor groups due to the rising levels of mental illness, shortage of therapists and treatment options.
According to the Centers for Disease Control and Prevention (CDC), the percent of adolescents reporting having a major depressive episode has increased by 60% between 2007 to 2019. The CDC data also reports that suicide rates among young people ages 10 to 24 climbed at a similar pace within the years 2007 to 2018.
Adolescents are undergoing a major change. Decades ago, the biggest health threats to teenagers in the US came from binge drinking, drunk driving, teenage pregnancy and smoking. These changes have been replaced by soaring rates of mental health disorders. “Young people are more educated; less likely to get pregnant, use drugs; less likely to die of accident or injury,” said Candice Odgers, a psychologist at the University of California, Irvine. “By many markers, kids are doing fantastic and thriving. But there are these really important trends in anxiety, depression and suicide that stop us in our tracks.”
Federal research shows that teenagers as a group are getting less sleep, less exercise and spending less time with friends in person. These things are all crucial for healthy development.
Are these issues inherent to adolescence that might have gone unrecognized before? Or are they being over diagnosed now? These are some of the questions posed as to why this surge is occurring. It is difficult to compare historical data around issues such as teen anxiety and depression because we only began collecting this data relatively recently. One thing that is certain, is that the rising rates of ER visits for suicide and self-harm show that the threat to mental health has changed significantly.
Sources: Matt Richtel. “It’s Life or Death’: The Mental Health Crisis Among US Teens,” The New York Times, 2022.General Health News
Unusual Cases of Hepatitis in Kids
Over the last year, hepatitis cases have been spiking amongst children. Twelve countries have reported at least 169 unusual cases of hepatitis in children, with the affected children ranging in age from one month to 16 years. Although most are younger than 10 years — and many are under 5 years. In one instance, seventeen of the children had undergone liver transplants due to hepatitis and at least one child died. Countries reporting hepatitis cases are the United Kingdom, Spain, Israel, Denmark and other European countries. In the United States, nine cases have been reported in Alabama, and two have been found in North Carolina. The initial cases in Alabama occurred in October and November of 2021. These cases were linked to adenovirus type 41 instead of the more typical hepatitis viruses labeled A through E. Adenovirus is a common virus that typically causes a cold or flu-like illness. All of the children were previously healthy at the time of hospitalization. The CDC does not know the cause or the number of cases and is working with state and local health departments to learn more about potential cases and what may be causing these illnesses. At this time, they believe that adenovirus could be the cause, but investigators are still learning more.
Sources: Helen Branswell. “WHO Says 12 Countries Have Reported Unusual Cases of Hepatitis in Kids,” STAT, 2022.Rising Number of Monkeypox Cases
The number of monkeypox cases is steadily rising in Europe and the US. So far, health officials have already traced the origin and spread of the monkeypox virus. Typically, people catch it from animals in West or Central Africa and import the virus to other countries. It actually does not come from monkeys. Instead, the virus likely persists in squirrels, pouched rats, dormice or other rodents. You can get monkeypox primarily from an animal bite, scratch or contact with the animal's bodily fluid. However, the virus can spread to other people through coughing and sneezing or contact with pus from the lesions. Community spread of monkeypox is currently suspected, and there is concern the virus may be spreading undetected, possibly through a new route of transmission.
So far, most of the cases are among men who have sex with men, but transmission can occur whether you are in the LBGTQ+ community or not. Monkeypox is a 2-to-4-week infection and can cause fever, body aches, enlarged lymph nodes and lesions that begin firm, deep-seated, bumpy and well-defined. Patients often develop a rash that progresses to small bumps on the skin, followed by blisters that may fill with whitish fluid. One version of monkeypox can be deadly, killing up to 10% of people infected. However, person-to-person transmission isn't common because it requires close contact with bodily fluids, such as saliva from coughing or pus from the lesions. Hence, the risk to the general population is low, the UK Health Security Agency (UKHSA) notes.
Sources: Michaeleen Doucleff. “Rare Monkeypox Outbreak in UK, Europe and US: What Is It and Should We Worry?,” NPR, 2022.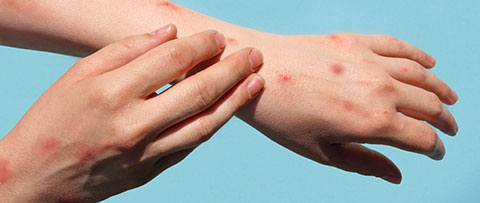
High-Cost Drugs
Bipartisan Lawmakers Advocate for Insulin Price Bill
As reported in 2019, about 37 million Americans, 11.3% of the total population, live with diabetes. This statistic includes almost 16 million seniors over the age of 65. With combined medical and pharmacy needs, people with diabetes spend, on average, 2.3 times more than those without diabetes.
The cost of diabetes medications, and insulin specifically, has understandably been a focus of several attempts to enact change with drug pricing bills. Earlier in the year, a group of bipartisan House and Senate lawmakers focused on limiting insulin costs as a major priority for Congress. Their discussions led to a release of a drafted bill that aims to lower insulin prices for diabetic members by capping copays at $35 or 25% of the list price. This proposal also included a measure to ensure member access to insulin products by removing barriers sometimes faced by prior authorizations or other “formulary management tools.”
This bill draft is designed to encourage lower list prices by also blocking the collection of rebates, which the proponents say are responsible for driving up the drugs’ costs. The Pharmaceutical Care Management Association (PCMA) has pushed back against the bill, specifically the rebate measure, saying that it would do little to actually lower costs for members and could “provide drug manufacturers additional opportunities to maximize revenues by gaming which products to roll back to 2006 prices to avoid discounting, and which products to keep at 2022 pricing.”
If list prices on insulins remain high, a copay cap of $35 might lower members’ out-of-pocket costs at the pharmacy counter. However, the plan sponsor/employer would be responsible for paying the remaining medication cost.
Similar proposals have been made and have stalled in the past. The Build Back Better Act included a $35 insulin cost cap as well, but it did not make it through the Senate last year after facing opposition. Previous attempts to remove rebates have also faced scrutiny and pushback with claims that their elimination could ultimately increase premiums for members.
Undoubtedly legislation will continue to look for ways to enact changes and lower drug costs for all, focusing on diabetes medications and insulin products. Plan sponsors can choose to design their benefits in a similar fashion even without a legislative requirement. For example, Express Scripts has a product called the Patient Assurance Program that caps patient copay at $25 for up to a 34-day supply of insulin products. Optum also offers a Critical Drug Affordability program that allows plans to set a copay of $0 – $25 for a 30-day supply of critical drug categories, including insulin.
Sources: Robert King. “Bipartisan Lawmakers Push for Ending Insulin Rebates in Drug Prices Bill,” Fierce Healthcare, 2022.ADA Staff. “Statistics About Diabetes,” American Diabetes Association, 2022.
Benita Lee. “How Much Does Insulin Cost? Here’s How 28 Brands and Generics Compare,” Good Rx Health, 2022.
Insulin Biosimilars with Higher Prices, PBMs and Payers
The goal of lowering prescription drug costs remains a top priority. One process that our prescription drug system already has in place to lower medication prices is to offer lower-cost alternative products like generics or biosimilars. Unfortunately, the drug pricing system in the US is not that straightforward. Increasingly, it seems that the pharmacy benefit managers (PBMs) are selecting products for their formulary with their lowest net cost, often reached with the list price discounts and rebates provided by the manufacturers. For some PBMs, their fees are calculated based on the list price of medication – that is, the price before discounts and rebates.
Plan sponsor clients may sometimes prefer the PBM to select these higher-priced products over the lower-priced versions because plan sponsors receive most of the rebates provided by manufacturers. Some employers use their rebates to offset overall healthcare costs and lower premiums for all their covered members.
“Some employers use their rebates to offset overall healthcare costs and lower premiums for all their covered members.”
There are scenarios in the industry where a higher-priced product may be preferred as a covered medication over a potentially lower-priced product because of the features our system ties to a drug’s price. This is one of the multitudes of factors that are being monitored ahead of Humira’s biosimilars that are anticipated to begin launching in 2023. Biosimilars being released for a top-selling medication like Humira is expected to have a profound impact on the industry as it operates today. However, what exactly that shakeup looks like is unknown. How the Humira biosimilars will be handled as they’re released in turn and how the market adapts to the competition are being closely monitored as it will be setting the stage for future biosimilar product launches.
Many questions are left circulating upon this pending release. Will the Humira biosimilars launch at list prices that are comparable to or higher/lower than Humira’s list price? Or will they launch with deep list price discounts to attempt to draw market share? How will the series of launches – and the pricing of the early releases – contribute to pricing strategies for those released later? Will the biosimilars released earlier have higher or lower list prices than the ones released later on? There are many potential scenarios, and things could change in the years following the initial product launches in response to market pressures and product competition.
Sources: Adam J. Fein. “Why PBMs and Payers Are Embracing Insulin Biosimilars with Higher Prices — And What That Means for Humira (Rerun),” Drug Channels, 2022.
Pharmacy and PBM News
Amazon Care Clinic Expansion
In 2019, Amazon first piloted its healthcare services with virtual urgent care provided for its own employees (and their families) in the Seattle, WA, area. It has since been rolled out to additional companies offering Amazon Care to their employees nationwide, including Silicon Labs, TrueBlue and Whole Foods Market. Eligible employees who live in cities where Amazon Care has in-person care services available have access to both virtual and in-person care services. In-person care is currently available in Seattle, Baltimore, Boston, Dallas, Austin, Los Angeles, DC and Arlington, Virginia. Amazon Care is working on expanding its blended care model to 20 new cities in 2022, including major metropolitan areas like San Francisco, Miami, Chicago and New York City.
In a press release, Amazon executives said its partner companies identified three key differentiators that stood out about their provided services:
- On-demand access to high-quality clinicians through Care Medical.
- Care Medical provides medical services for the app-based Amazon Care.
- Services include video care, in-app text chat with clinicians, mobile care visits, prescription delivery from a care courier and in-person care (Amazon Care can dispatch a medical professional to a patient’s home for services ranging from routine blood draws to listening to a patient’s lungs).
- Amazon Care’s comprehensive services model.
- Amazon Care offers access to urgent and primary care services, including COVID-19 and flu testing, vaccinations, treatment of illnesses and injuries, preventive care, sexual health and prescription requests and refills.
- A seamless patient experience.
- Amazon Care has a patient satisfaction rating of 4.7 out of 5.
Prime Therapeutics Acquires Magellan Rx
In 2021, Centene announced that it would acquire Magellan Health and that the $2.2 billion deal officially closed in January 2022. In May, it was announced that Prime Therapeutics would be acquiring the pharmacy line of Magellan Health, known as Magellan Rx Management. This $1.35 billion deal is expected to close by the end of 2022.
“This is a timely and important move,” said Ken Paulus, CEO and president of Prime Therapeutics. “As pharmacy costs balloon, bold action is necessary. By bringing together the capabilities and talents of Prime and Magellan Rx, we are positioned to deliver breakthrough value to the clients and members we serve. We are excited about the solutions our shared teams will bring to the industry as we strive to deliver progress against the Quadruple Aim.”
Often, industry acquisitions such as this occur so that companies can share each other’s strengths rather than expend unnecessary resources to replicate a proven model. Magellan Rx has nearly two decades of specialty drug management expertise managing complex patient populations across both the pharmacy and medical benefits, serving more than 16 million members. Magellan Rx also has expertise with Medicaid and state pharmacy program administration solutions. As for now, Magellan Rx will continue to operate as a stand-alone business unit under Prime’s umbrella to enable continuity with its current customers, while adding the value of its solutions to Prime’s plan sponsors.
Source: Jenine Anderson. “Prime Therapeutics Is Acquiring Magellan Rx to Advance Integrated Specialty Drug Management, Accelerating Efforts to Lower the Cost of Drugs and Improve Health Outcomes,” Prime Therapeutics, 2022.Delayed Telehealth Adderall Prescriptions
Over the years, telehealth has been a steadily growing area, and the pandemic seems to have accelerated its utilization. Overall, the telehealth segment and associated services have been a great resource for patients. While a lot of members have gone back to their traditional care model, the mental health category still has a large focus and usage of telehealth.
This being said, it appears that some of the telehealth companies may not be operating in the best interest of the patients, and even the retail pharmacies are questioning the validity of the prescription orders. Specifically, prescriptions for medications like Adderall and other similar stimulants, which the federal government classifies as a controlled substance due to underlying abuse, potentially appear to be over-prescribed.
There are reports of major retail pharmacies, including Walgreens, CVS and Walmart, who have all blocked or delayed questionable prescriptions from online mental health-focused organizations, including Done and Cerebral. The telehealth companies point towards a lack of understanding around policy which is not an isolated problem. The larger, more established telehealth companies such as Teladoc Health Inc., American Well Corp., MDLive, and Included Health do not even prescribe these kinds of controlled medications via telehealth visits.
Stimulant medications like Adderall can be beneficial for patients with attention deficit hyperactivity disorder (ADHD), and a lot of patients are managed well with these medications. The questions come in when evaluating if a true diagnosis can be made for ADHD in the limited timeframe of a telehealth visit. Previously, Done and Cerebra prescribers have stated feeling pressure to write for these types of medications.
IQVIA has reported significant increases (10.4% from 2020) in prescriptions like Adderall being filled in the United States, which falls in line with telehealth companies like Done and Cerebral pushing for more of these orders to be written. There are a number of reasons why a pharmacy would not be able to complete the fulfillment of a prescription order. Still, it is clear there are several large pharmacy chains taking precautions to prevent over-prescribing.
Source: Rolfe Winkler and Sarah Nassauer. “Walmart, CVS Pharmacies Have Blocked or Delayed Telehealth Adderall Prescriptions,” The Wall Street Journal, 2022.
Uncovering Digital Pharmacies
Digital pharmacies are a rapidly growing segment. They combine the prescriber piece of getting the order and the pharmacy piece of filling the prescription. Being technology driven is a fundamental piece to the puzzle as the majority of the leading digital pharmacies utilize a mobile app as their primary method of patient interaction. The members can order prescriptions, schedule delivery, manage their accounts or potentially set up telehealth consults via digital platforms.
The business models will have some variation, but most of the digital pharmacies will have at minimum, one physical location so the pharmacy can be in a PBM network and usually focus on thirty-day prescriptions. Some will be more aligned towards a smaller formulary and cash pay format where the members’ insurance is not used, but it will often be dependent on the telehealth company the pharmacy is aligned with. Some of the companies have a large focus on areas such as sexual health, hair loss and smoking cessation.
There are a number of smaller digital pharmacies, and while they are not yet making a big splash in the competitive pharmacy market, they are getting a lot of interest from investors. Additionally, bigger established pharmacy chains are interested in the technology provided by some of these companies and instead of trying to create it on their own, they are buying them. For example, Walmart purchased CareZone’s digital prescription technology, OptumRx bought DivvyDose and Target picked up Deliv Rx.
As we have seen the increased use of telehealth, it would seem like a natural progression for digital pharmacies to become more heavily utilized. As the digital pharmacies become more integrated with PBMs and the major retailers enter this space, it is possible digital pharmacy opportunities could expand beyond a few niche disease states.
Source: Adam J. Fein. “The Promise and Limits of Digital Pharmacies,” Drug Channels, 2022.Labor, Benefits and Legislation
When Inflation Impacts Health Benefits
With inflation on the rise, chief financial officers (CFOs) are concerned about the cost of health benefits impacting their organization’s sustainability. The second largest HR expense, behind employee salaries, is health benefits. Some of the CFOs’ top concerns include higher utilization due to "catch-up" care or avoided care during the pandemic, claims for long COVID-19, and new gene and cellular therapies. Healthcare costs have increased year over year, however, we most likely have not seen the impact of inflation for a few years due to contracts that lock in pricing. Another challenge for CFOs during the “Great Resignation” is finding a balance between expenses and personnel retention. Most CFOs emphasized that clinical management programs should be prioritized over changes to the plan design, which typically shift expenses to employees, increasing the likelihood that they would be dissatisfied. In the future, it will be crucial for the finance department and benefits personnel to communicate more. Businesses must prepare for the worst and take action to slow cost growth.
Source: Alan Goforth. “Buckle Your Seatbelts: CFOs Fear Impact of Inflation on Health Benefits Costs,” BenefitsPRO, 2022.Medicaid Copay Accumulator Rule
Centers for Medicare and Medicaid Services’ Best Price Rule addressed concerns over accumulator adjustment programs – called copay accumulator or maximizer programs – put in place by insurers and their PBMs. These programs prevent the copay assistance offered by drug manufacturers from accumulating towards members’ deductibles and out of pockets. The rule proposed changes to the Medicaid drug rebate program (MDRP) policies to encourage manufacturers to ensure copay assistance programs would directly benefit members. However, it could not get around the PBM accumulator adjustment programs in the timeframe allowed. For now, the rule will not go into effect but it could be appealed.
Source: Adam J. Fein. “How the Medicaid Copay Accumulator Rule Will Hurt Prescription Affordability,” Drug Channels, 2022.Jeffrey I. Davis, et al. “Federal District Court Vacates Copay Accumulator Adjustment Rule: Programs Remain the Same for Now,” Bass, Berry & Sims PLC.
Health Can’t Wait
Over three years ago, a coalition, Health Can’t Wait, was formed to help prevent delayed access to essential healthcare services via legislation. Michigan State Medical Society (MSMS) physicians and partners described many stories of how prior authorizations caused delays and interfered with medical decision-making. Eventually, in April 2022, Governor Gretchen Whitmer signed Senate Bill 247, which streamlines medical offices' interactions with payers, leading to shorter wait times for prior authorizations and less paperwork, which will eventually improve patient access to care. According to MSMS, Senate Bill 247 would reform the prior authorization process to add requirements around steps PBMs must take to notify providers and members of changes, as well as specify timeframes for a response and consequences of non-response. Even though many of these provisions are already PBM common practices, this bill could help to standardize the industry processes if it catches on in other states.
Source: MSMS Staff. “Prior Authorization Reform Has Been Signed into Law,” Michigan State Medical Society, 2022.
